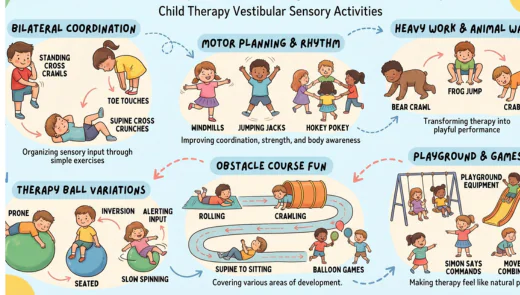
Child Therapy Vestibular Sensory Activities. Vestibular sensory input serves as a powerful tool when helping children with sensory needs, creating long-lasting effects on each individual’s natural development.
From the moment infants are exposed to movement, it promotes healthy development and integration across multiple systems movement activates the vestibular system during everyday participation in tasks like dance, spinning, kneeling on knees, laying on the couch, crawling, standing on a ladder, resting on the belly to read a book, walking on tiptoes, performing somersaults, navigating monkey bars, going up or down stairs, bouncing on a trampoline, riding an elevator, driving down a hill in a car, sliding on a sled, or rocking in a rocking chair.
These movements can make us feel calm, alert, wired, or relaxed. Sometimes,our hands sweat just thinking about heights, or the thought of a roller coaster makes us queasy, demonstrating how movements impact the way we feel and how movements impact behavior.
How the Vestibular System Works
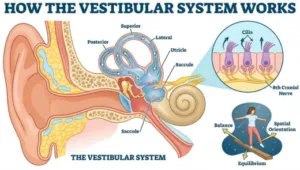
Child Therapy Vestibular Sensory Activities. The vestibular system, housed within the inner ear, operates through semicircular canals and otolith organs that detect rotary movements, linear acceleration, and changes in head position across three-dimensional space.
This sensory processing mechanism relies on microscopic hair cells that respond to acceleration, deceleration, and gravity, sending signals via the 8th cranial nerve to help maintain equilibrium and spatial orientation.
Understanding how these vestibular apparatus components work together, the three circular shapes positioned in different planes alongside the cochlea, reveals why vestibular sensory processing affects everything from balance to how we interact with our surroundings, making it essential for daily function and occupational performance in both familiar and unfamiliar spaces.
Types of Movement the Vestibular System Senses
Child Therapy Vestibular Sensory Activities. In therapy work with children, understanding that vestibular input operates through distinct movement patterns becomes crucial for therapists designing activities that target specific sensory needs.
The inner ear receptors within semicircular canals respond to angular movements like spinning and head rotation, while otolith organs detect linear movement such as forward-back rocking or vertical jumping on trampolines.
Rotary movements through spinning equipment, horizontal swinging back and forth, upside-down inversion with head positioning changes, and challenges involving height or balance on uneven surfaces each activate different vestibular pathways that impact coordination, motor planning, and spatial orientation.
Therapists must consider how seated, prone, standing, or supine positions during activities affect vestibular system processing, since combining lateral movements with changes in speed, direction, or body positioning creates varied sensory input that can calm or alert the nervous system depending on individualized needs.
How Vestibular Input Relates to Interoception
The connection between vestibular input and interoception reveals how movement directly impacts our body’s ability to recognize internal states. When children engage in spinning, jumping, or swinging activities, their vestibular system simultaneously triggers awareness of heart rate, breathing patterns, and muscle tension.
Receptors in the inner ear send signals that integrate with somatosensory information, helping kids discern whether they feel calm or alert, ultimately supporting self-regulation as they learn to respond appropriately to their body’s cues.
Child Therapy Vestibular Sensory Activities must incorporate this bidirectional sensory relationship, which explains why rocking, rolling, or even head position changes can help children who struggle with attention, arousal levels, or emotional disorientation to reset their internal monitoring systems.

Vestibular Processing Disorders and Red Flags
Child Therapy Vestibular Sensory Activities. When children struggle with vestibular processing, the red flags often surface through difficult maintaining balance during movement activities or exhibiting fearful responses to playgrounds, stairs, and swings. You might notice fidgeting, moving constantly, or conversely,a fear of falling that leads to slouching, leaning against desks and tables for stability.
These challenges can manifest as gravitational insecurity, where typical movement patterns feel threatening, or as excessive sensory-seeking behaviors like constant spinning, jumping, or hanging upside down to satisfy an under-responsive vestibular system.
What’s particularly telling is when equilibrium issues impact daily function, making simple tasks like walking or sitting in standing positions exhausting, while rotary movements or heights trigger intense visceral response where the stomach rolls, and hands sweat, clear signs the interoceptive system is activating in tandem with vestibular distress.

Activities to Regulate the Vestibular System
When nervous systems become constantly inundated with sensory input, the body’s internal responses shift toward overload, pupil dilation, sweaty palms, and changes in respiration. I’ve witnessed how slowly rocking in a hammock or gentle lateral movements on sensory swings can calm an overstimulated child down, essentially using the same vestibular system that triggered distress to restore equilibrium.
The interoceptive system is simultaneously activated during these calming movements, which helps children become aware of internal feelings like body temperature and heart rate, creating a feedback loop where motion becomes medicine rather than mayhem.
What’s fascinating is how slow swinging in a prone position on platform swings or lycra swings can normalize a child’s tactile defensiveness while addressing gravitational insecurity. Theplay therapy for kids essentially treats multiple sensory systems through one activity.
These vestibular input activities must be carefully monitored, as what appears calming during the actual activity might trigger negative reactions several hours after the therapy session, making it important to use extreme caution and never exceed the 10-minute threshold for intense rotary movements or inversion types.

Vestibular Movement Ideas to Try
Child Therapy Vestibular Sensory Activities. When children struggle with sensory processing disorder, incorporating movement into their daily activities becomes essential for organizing sensory input. Bilateral coordination develops naturally through simple vestibular exercises like standing cross crawls, toe touches, and supine cross crunches, while jungle animal heavy work coordination exercises and animal walks transform therapy interventions into playful ways that promote performance.
Motor planning improves when kids engage in windmills, jumping jacks, and hokey pokey, which address multiple skills simultaneously: coordination, strength, body awareness, and position in space, making these movement-based activities a valuable tool for seeking vestibular input. Obstacle courses remain a great way to cover various areas of development, especially when listed activities include rolling, crawling, supine to sitting motions, sitting to side lying motions, and balloon games that require core strength and balance.
Therapists often work with therapy ball variations where children lie down in a prone position or seated, adding inversion and slow spinning elements that support the sensory input needed for alerting the system.
Head and neck movements, tilting side to side with anteroposterior movements, basically serve as body position changes that create vestibular input through integration of sensory systems (visual, tactile, proprioceptive, vestibular), and it’s pretty cool how these work together in an integrated manner during movement and activity.
Playing with playground equipment, Simon Says Commands, and movement combinations helps improve while making therapy sessions feel less clinical and more like natural play.
Vestibular Safety: Risks and Contraindications
When implementing in child Therapy Vestibular Sensory Activities in child therapy vestibular sensory activities, awareness of individual tolerance levels must guide every session. Some children experiencing dizziness, vertigo, or lightheadedness may signal vestibular disorders requiring clinical evaluation before continuing movement-based interventions.
Fatigue, persistent headaches, or a spinning room sensation during swinging, trampolines, or inverted head positioning often indicate inner ear issues or auditory nerve impairment that impact balance and equilibrium. Rather than pushing through difficulties, consider stopping immediately when red flags emerge, particularly with children who demonstrate poor spatial awareness, visual processing problems, or adjusting challenges against gravity.
Depending on the severity, seeking out a therapist specializing in vestibular therapy becomes essential for addressing underlying concerns through specific vestibular exercises designed for acute setting needs.

Therapeutic and Sensory Swings for Vestibular Support
In therapy work, sensory swings remain a goldmine for addressing vestibular challenges that often arise from poor integration of movement and balance. The single-hung point design of these suspended tools allows for linear, rhythmic swinging that can last up to 8 hours in its calming effect on the central nervous system, making them ideal for children who cannot fall asleep or concentrate during tedious tasks.
Equipment like pod swings and cocoon-style seats provides proprioceptive input while the person experiences gentle, slow motions that help inhibit the reticular activating pathways, a powerful way to encourage self-soothing without overload.
When incorporated into sensory integration sessions, these swings serve as both organizing and alerting mechanisms for speech delay activities, though practitioners should keep in mind that spinning should be closely monitored for individuals with seizures or high blood pressure, as vestibular input can trigger reactions that occur long after the activity has ended.
Home-Based Vestibular Activity Ideas
When everyday objects transform into therapeutic tools, the home becomes an extension of the clinic. A laundry basket filled with pillows creates an unstable surface for sitting and balance work, while couch cushions arranged in a path challenge motor planning as children crawl across uneven terrain.
Child Therapy Vestibular Sensory Activities. Blanket swings suspended from doorway bars offer linear motion that produces calming input, and a mattress propped against the wall becomes a ramp for rolling activities. Household items like yoga balls, rope tied between furniture for obstacle courses, and even cardboard boxes for tunnels provide rich vestibular stimulation without requiring extensive equipment lists.
The Playground as a Sensory Integration Tool
Child Therapy Vestibular Sensory Activities. Outdoor playground climbing structures offer rich opportunities for vestibular input through slides, swings, and monkey bars that stimulate the inner ear apparatus while children ride, jump, and spin.
The ground beneath their feet constantly changes from foam surfaces to tire bounce zones, activating muscle and joint receptors that contribute to postural adjustments and spatial orientation as kids climb slopes, hop like a frog, or go down steep pathways.
I’ve noticed how even simple outdoor activities like stepping stone paths or walking narrow beams facilitate equilibrium development, integrating visual-motor skills with movement participation in ways that indoor sessions sometimes struggle to replicate. The world around them becomes an active tool for sensory processing, where motions feel natural rather than clinical.
Conclusion
When vestibular therapy becomes part of daily functional life, the brain naturally integrates these sensations without the child actively thinking about posture or balance. Benefits emerge through play rather than clinical drills, whether it’s a friend pushing them on a swing or going down a slide at the playground.
Child Therapy Vestibular Sensory Activities. The real work happens when movements become typical parts of their routine, allowing coordination and body awareness to develop through games, outdoor activities, and even household obstacle course challenges that address processing deficits while building confidence in unfamiliar spaces.
FAQs About Vestibular Sensory Activities in Child Therapy
What’s the quickest way to calm a child’s vestibular system when they’re overwhelmed?
Forward-back rocking in a hammock or porch swing for about 15 minutes provides the longest lasting impact on system regulation, especially when coupled with low-frequency sounds – this effective tool works best first thing in the morning or afternoon rather than night since fast vestibular input can make sleeping difficult for some children.
Can vestibular activities help with issues beyond just movement coordination?
The vestibular system operates in conjunction with interoception, meaning children who struggle to tolerate roller coasters often have trouble negotiating hunger, thirst, and internal body signals – impacting their ability to participate in social interaction and maintain alertness throughout the day, which is why ongoing therapy addresses both sensory-seeking and sensory-avoiding responses through appropriate movement plans.
What precautions should therapists consider when adding vestibular input to treatment sessions?
Vestibular input is extremely powerful and not always apparent – children with impaired systems can appear to respond well initially but then experience delayed reactive responses including throwing up, eye tracking problems, or changes in blood pressure following a treatment session, so small amounts administered in 30-45 minute breaks with visual monitoring definitely cover safety precautions rather than pushing children who have reached their threshold.
How do playground structures provide natural vestibular therapy opportunities?
Playgrounds built with monkey ladder bars, ramps, slides, and merry-go-round equipment offer different planes of motion – lying prone on a swing in superman position requires core strength and neck extension while scooting sideways across beams challenges lateral coordination, and even old school structures like picnic bench steps or unoccupied parallel bars become effective tools when therapists show children how to use their body’s weight for resistance training.
What household items can families use to create vestibular activities at home?
An office chair that swivels becomes a disc for rotary input, masking tape creates hopscotch patterns for jumping sequences, bubble wrap under a wobble disk adds tactile feedback to balance work, while a couch transforms into a crash space for prone rolls and somersaults – families can make a rope beam on the floor, try animal walks up stairs, or hold a blanket like a hammock to rock younger children back and forth, giving parents ways to support their child’s vestibular diet needs without using expensive equipment from occupational therapy clinics.